Osteoporosis is often called the “silent disease” because it progresses without symptoms until a fracture occurs. Among the different types, postmenopausal osteoporosis is particularly significant. It affects millions of women worldwide, severely impacting their health, independence, and quality of life. Understanding this condition is crucial for early intervention and prevention.
Postmenopausal osteoporosis is a form of osteoporosis that develops after menopause. It is characterized by a decrease in bone mass and density, making bones more fragile and susceptible to fractures. Menopause marks the end of a woman’s menstrual cycles and is accompanied by a sharp decline in estrogen levels, a hormone that plays a vital role in maintaining bone strength.
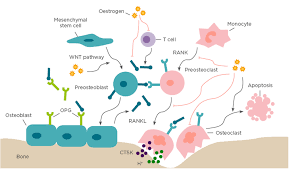
Without enough estrogen, the balance between bone resorption (breakdown) and bone formation shifts. Bone is broken down faster than it is rebuilt, leading to porous, weakened bones.
Causes and Risk Factors
The primary cause of postmenopausal osteoporosis is the drop in estrogen production following menopause. However, several factors can increase a woman’s risk, including:
- Genetics: A family history of osteoporosis can predispose someone to the disease.
- Body Frame Size: Women with smaller, thinner frames tend to have a higher risk.
- Age: Bone loss accelerates with age, especially after the age of 50.
- Lifestyle Factors: Smoking, excessive alcohol consumption, poor nutrition, and lack of physical activity can all contribute to bone loss.
- Medications: Long-term use of corticosteroids and certain other drugs can weaken bones.
- Medical Conditions: Disorders like rheumatoid arthritis, thyroid diseases, and gastrointestinal conditions that affect nutrient absorption can increase osteoporosis risk.
Symptoms and Complications
Early stages of osteoporosis are typically symptomless. Many women do not realize they have it until they suffer a fracture, often in the hip, spine, or wrist. Other signs may include:
- Loss of height over time
- A stooped posture
- Back pain caused by fractured or collapsed vertebrae
Fractures resulting from osteoporosis can lead to chronic pain, disability, and a significant loss of independence, making it a major public health concern.
Diagnosis
Postmenopausal osteoporosis is typically diagnosed through a bone mineral density (BMD) test, commonly known as a DEXA scan. This painless test measures the density of bones, often at the hip and spine, to determine the risk of fractures.
Physicians may also assess risk factors and medical history to guide diagnosis and treatment decisions.
Prevention and Management
The good news is that postmenopausal osteoporosis can often be prevented or managed effectively. Strategies include:
Lifestyle Changes
- Nutrition: A diet rich in calcium and vitamin D is essential for bone health. Dairy products, leafy greens, fortified foods, and supplements can help meet daily requirements.
- Exercise: Weight-bearing and strength-training exercises stimulate bone formation and improve balance, reducing the risk of falls and fractures.
- Avoid Tobacco and Limit Alcohol: Both can weaken bones and should be minimized or avoided.
Medications
Several medications are available to treat osteoporosis, including:
- Bisphosphonates: These drugs slow bone loss and are commonly prescribed.
- Hormone Replacement Therapy (HRT): While effective for some women, HRT carries risks and is usually considered on an individual basis.
- Selective Estrogen Receptor Modulators (SERMs): These mimic estrogen’s positive effects on bone density.
- Anabolic Agents: Newer medications that stimulate bone formation may be recommended for those with severe osteoporosis.
Regular Monitoring
Follow-up bone density tests and regular consultations with healthcare providers help monitor progress and adjust treatments as needed.
Conclusion
Postmenopausal osteoporosis is a serious but manageable condition. Early awareness, proactive lifestyle changes, and appropriate medical intervention can significantly reduce the risk of fractures and maintain quality of life. Empowering women with the knowledge and tools to protect their bone health is a vital step toward healthier aging.
The list of some Postmenopausal Osteoporosis medicine:
Estracon
Rozy
Rozy DS