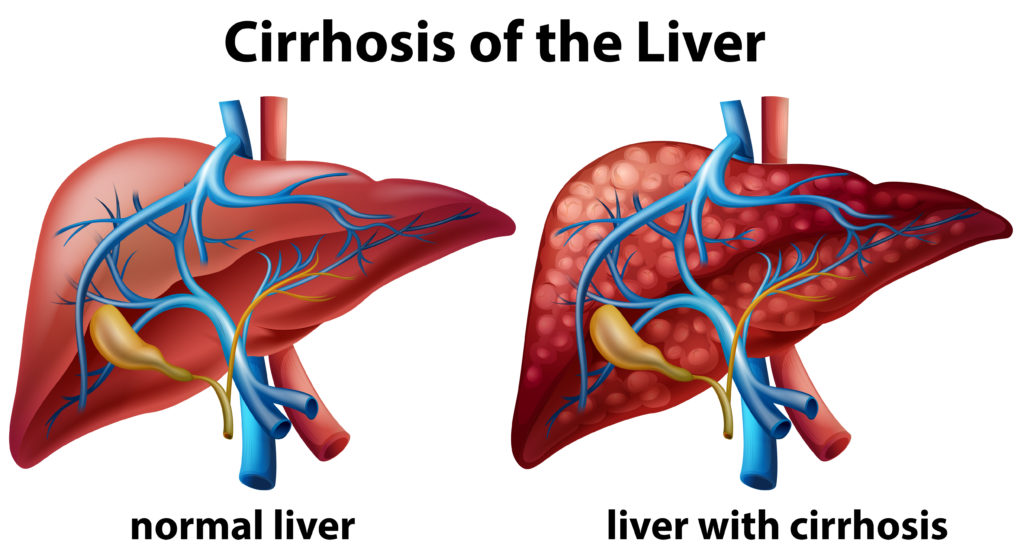
The liver is a powerhouse organ that plays a vital role in digestion, detoxification, and nutrient storage. However, when it’s repeatedly injured — whether by infection, toxins, or chronic health conditions — it can gradually become scarred and damaged. This progressive scarring is known as liver cirrhosis, a serious and often irreversible condition that can severely affect a person’s health and quality of life.
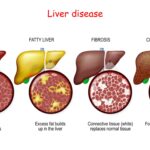
Liver cirrhosis occurs when healthy liver tissue is replaced by scar tissue (fibrosis), blocking the normal flow of blood through the liver and impairing its function. As scar tissue accumulates, the liver loses its ability to perform essential tasks, such as filtering toxins, producing vital proteins, and regulating blood clotting.
Cirrhosis typically develops over many years and often remains silent until significant liver damage has occurred.
Causes of Liver Cirrhosis
Several conditions and behaviors can lead to liver cirrhosis, including:
- Chronic Alcohol Abuse: Excessive, long-term alcohol consumption is one of the most common causes.
- Chronic Viral Hepatitis: Hepatitis B and C infections can cause ongoing inflammation, leading to scarring.
- Non-Alcoholic Fatty Liver Disease (NAFLD): Accumulation of fat in the liver, often associated with obesity, diabetes, and high cholesterol, can progress to cirrhosis.
- Autoimmune Hepatitis: The body’s immune system mistakenly attacks liver cells.
- Biliary Diseases: Conditions such as primary biliary cholangitis or primary sclerosing cholangitis affect bile ducts and can lead to cirrhosis.
- Genetic Disorders: Conditions like hemochromatosis (excess iron accumulation) and Wilson’s disease (copper buildup) can damage the liver over time.
- Long-Term Drug or Toxin Exposure: Some medications or toxins can cause chronic liver injury.
Symptoms of Liver Cirrhosis
In the early stages, cirrhosis may not produce noticeable symptoms. As the disease advances, symptoms can include:
- Fatigue and weakness
- Easy bruising and bleeding
- Swelling in the legs, ankles, or abdomen (edema and ascites)
- Jaundice (yellowing of the skin and eyes)
- Itchy skin
- Loss of appetite and weight loss
- Confusion, memory problems, and personality changes (hepatic encephalopathy)
- Spider-like blood vessels on the skin (spider angiomas)
Advanced cirrhosis can lead to life-threatening complications like liver failure and liver cancer.
Diagnosis of Liver Cirrhosis
Diagnosing cirrhosis typically involves:
- Physical Examination: Checking for signs like jaundice, swelling, or spider angiomas.
- Blood Tests: Assess liver function and look for abnormalities in blood counts or clotting.
- Imaging Studies: Ultrasound, CT scans, or MRI can reveal liver size, structure, and signs of portal hypertension.
- Liver Biopsy: In some cases, a small tissue sample is taken to confirm the extent of scarring.
- Elastography: A non-invasive test that measures liver stiffness to assess fibrosis severity.
Early diagnosis is crucial for managing the disease and preventing complications.
Treatment and Management
While the damage caused by cirrhosis is often permanent, treatment focuses on slowing progression, managing symptoms, and preventing complications:
- Addressing the Underlying Cause: Stopping alcohol consumption, treating hepatitis infections, controlling blood sugar levels in diabetes, and managing obesity can halt or slow further liver damage.
- Medications: Drugs can control hepatitis infections, reduce portal hypertension, and manage symptoms like itching or confusion.
- Lifestyle Changes: Eating a healthy diet low in salt, avoiding alcohol, and maintaining a healthy weight are essential.
- Monitoring for Complications: Regular screenings for liver cancer and routine check-ups are vital.
- Liver Transplant: For individuals with end-stage liver disease, a liver transplant may be the only option for survival.
Close cooperation with healthcare providers, including hepatologists, nutritionists, and primary care doctors, is key to managing cirrhosis effectively.
Preventing Liver Cirrhosis
Prevention plays a significant role in reducing the burden of liver disease. Steps include:
- Moderating or eliminating alcohol intake
- Getting vaccinated against hepatitis A and B
- Practicing safe hygiene and avoiding sharing needles to reduce hepatitis transmission
- Maintaining a healthy weight
- Managing chronic health conditions like diabetes and high cholesterol
Simple lifestyle choices can protect the liver and prevent the slow march toward cirrhosis.
Conclusion
Liver cirrhosis is a serious but often preventable disease. Recognizing risk factors early, seeking timely treatment, and making healthy lifestyle changes can make a profound difference in disease progression and quality of life. As awareness grows and treatments advance, there is hope for better outcomes and a healthier future for those at risk.
The list of some Liver Cirrhosis medicine:
Heparest