Leiomyosarcoma (LMS) is a rare type of soft tissue sarcoma that originates in smooth muscle cells. These are the involuntary muscles found in organs such as the stomach, intestines, blood vessels, and the uterus. Unlike other common tumors, leiomyosarcoma is malignant, meaning it can grow rapidly and spread to other parts of the body.
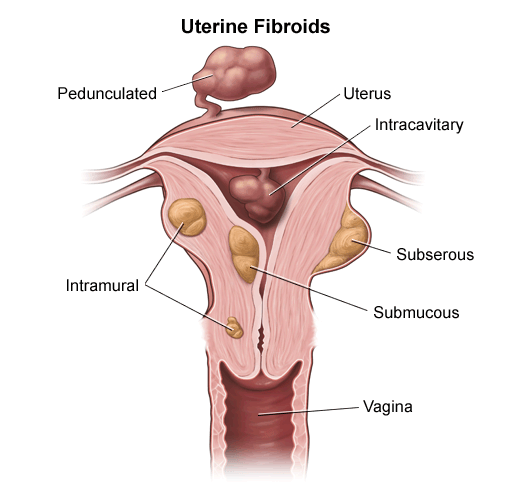
Though leiomyosarcoma can develop anywhere smooth muscles are present, it most commonly arises in the uterus, abdomen, or blood vessel walls.
Causes and Risk Factors
The precise cause of leiomyosarcoma remains unclear. However, several factors may increase the risk of developing this cancer:
- Radiation exposure: A history of radiation therapy, especially for previous cancers, can raise the risk.
- Genetic syndromes: Conditions such as Li-Fraumeni syndrome and hereditary retinoblastoma are linked to higher sarcoma risks.
- Chemical exposure: Contact with certain industrial chemicals might play a role, although this is less proven.
- Spontaneous occurrence: Many cases arise without any known cause or prior risk factors.
Leiomyosarcoma is more frequently diagnosed in adults, typically between the ages of 40 and 60, and is slightly more common in women, especially when it develops in the uterus.
Symptoms of Leiomyosarcoma
The symptoms vary based on the tumor’s location and size. Early stages often do not cause noticeable problems, but as the tumor grows, symptoms may appear, such as:
- A painless lump or swelling in soft tissues
- Abdominal pain or bloating
- Unexplained weight loss
- Fatigue
- Changes in menstrual bleeding (if the uterus is affected)
- Blood in the stool or urine (if near gastrointestinal or urinary organs)
Because the signs are often subtle at first, leiomyosarcoma may not be diagnosed until it reaches a more advanced stage.
Diagnosis
Diagnosing leiomyosarcoma typically involves multiple steps:
- Imaging tests: MRI or CT scans help locate the tumor, assess its size, and check for possible spread.
- Biopsy: A tissue sample is taken and examined under a microscope to confirm the diagnosis and differentiate it from other tumors.
- Blood tests: While they do not diagnose LMS directly, they can help evaluate overall health and organ function before treatment.
Accurate diagnosis is crucial since treatment plans depend heavily on the tumor’s grade, size, and whether it has metastasized.
Treatment Options
Treatment for leiomyosarcoma is often aggressive due to its malignant nature. Main approaches include:
- Surgery: Removing the tumor with wide margins of healthy tissue is the primary treatment. In some cases, complete removal may not be possible if the tumor is near vital organs.
- Radiation therapy: Often used before or after surgery to shrink the tumor or kill remaining cancer cells.
- Chemotherapy: Especially important if the cancer has spread (metastasized) or cannot be completely removed with surgery. Doxorubicin and ifosfamide are commonly used drugs.
- Targeted therapy: Some newer treatments aim at specific mutations within cancer cells, offering potential options for advanced cases.
A multidisciplinary team usually manages leiomyosarcoma, combining surgical, medical, and radiation oncology expertise.
Prognosis
The outlook for leiomyosarcoma varies depending on:
- The tumor’s size and location
- How early it is detected
- Whether it has spread to other parts of the body
- The tumor’s grade (how aggressive the cancer cells appear)
Generally, smaller, localized tumors that can be fully removed surgically offer a better prognosis. Unfortunately, leiomyosarcoma has a high tendency to recur, even after successful treatment, making long-term follow-up critical.
Conclusion
Leiomyosarcoma is a serious and rare cancer that demands prompt diagnosis and aggressive treatment. Advances in surgical techniques, chemotherapy, and targeted therapies are improving outcomes, but early detection remains key. If you experience unexplained lumps, persistent pain, or other unusual symptoms, seeking medical advice early can make a significant difference.
The list of some Leiomyosarcoma medicine:
Yondelis