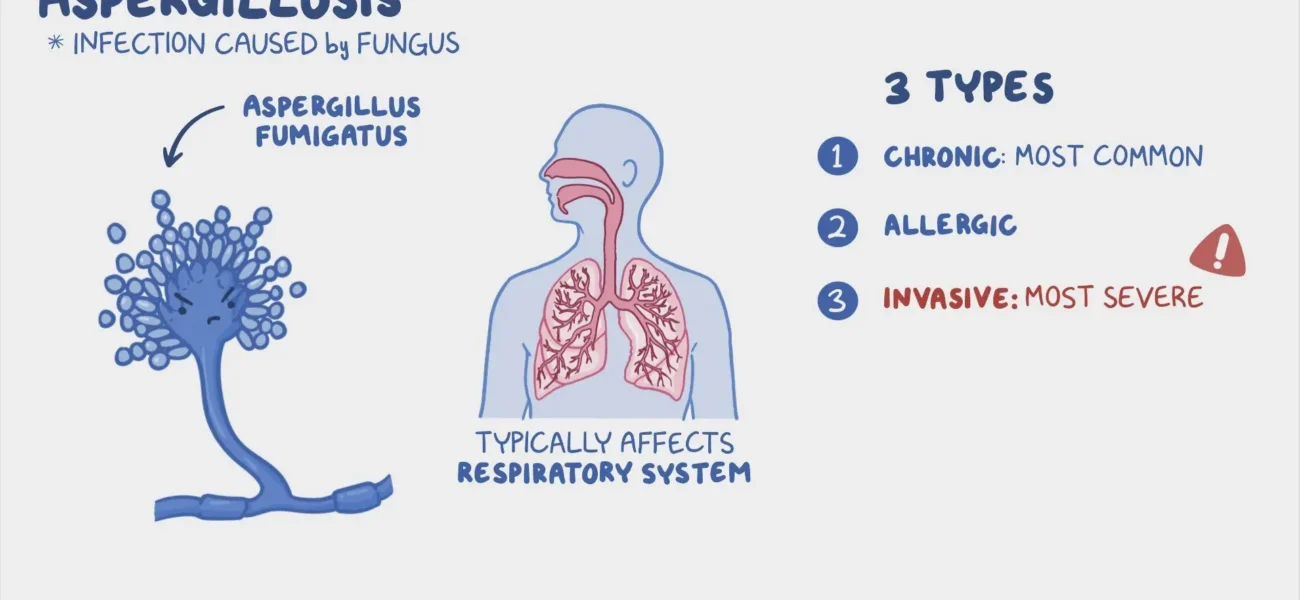
Invasive aspergillosis occurs when Aspergillus fungi invade the body’s tissues, often the lungs, and cause an infection. The most common species responsible for invasive infections are Aspergillus fumigatus, although other species, like Aspergillus flavus and Aspergillus niger, can also be involved.
In healthy individuals, the body’s immune system is typically able to prevent the fungi from causing harm. However, in people with compromised immune systems—such as those undergoing chemotherapy, organ transplant recipients, or individuals with chronic lung diseases—the fungi can invade deeper tissues, leading to more severe and invasive infections.
In this blog, we will explore what invasive aspergillosis is, who is at risk, its symptoms, diagnosis, treatment options, and how it can be prevented.
How Does Invasive Aspergillosis Develop?
Aspergillus fungi are omnipresent in the environment, often present in soil, dust, and decaying organic matter. These fungi release microscopic spores (conidia) that can be inhaled into the lungs. In people with healthy immune systems, these spores are usually cleared without causing illness. However, in individuals with weakened immune defenses, the spores can invade the lung tissue and other organs.
When inhaled, the spores settle in the lungs, where they can cause inflammation and tissue damage. Invasive aspergillosis can rapidly spread to other parts of the body, such as the sinuses, brain, heart, kidneys, and liver, depending on the severity and location of the infection.
Risk Factors for Invasive Aspergillosis
Several factors increase the likelihood of developing invasive aspergillosis, including:
- Weakened immune system: Conditions such as leukemia, lymphoma, HIV/AIDS, and other immunocompromising diseases increase the risk.
- Organ transplantation: Those who have received organ transplants (e.g., kidney, heart, lung, or liver transplants) are at a higher risk due to the use of immunosuppressive drugs.
- Chemotherapy and radiation therapy: Cancer patients undergoing chemotherapy or radiation therapy for cancer treatment are at significant risk because these treatments weaken the immune system.
- Chronic lung diseases: Conditions like chronic obstructive pulmonary disease (COPD), cystic fibrosis, or tuberculosis can make the lungs more vulnerable to infection.
- Corticosteroid use: Prolonged use of corticosteroids can suppress the immune system, making it easier for Aspergillus fungi to infect the body.
Additional Risk Factors Include:
- Severe neutropenia (low white blood cell count)
- Blood disorders
- Diabetes
- Previous infections or trauma
Because of these risk factors, individuals with compromised immunity are the primary population affected by invasive aspergillosis.
Symptoms of Invasive Aspergillosis
The symptoms of invasive aspergillosis can vary depending on the affected organs, but common symptoms include:
- Fever: Persistent or high-grade fever, often unresponsive to antibiotics.
- Coughing: A persistent cough, which may be dry or productive (with sputum).
- Chest pain or tightness: Pain in the chest due to lung involvement.
- Shortness of breath: Difficulty breathing, especially with exertion.
- Fatigue: Extreme tiredness, even with minimal physical activity.
- Sinus symptoms: Headache, facial pain, and sinus congestion if the infection involves the sinuses.
- Blood in sputum: In more severe cases, coughing up blood or blood-stained mucus.
- Neurological symptoms: If the infection spreads to the brain, symptoms can include confusion, seizures, or altered mental status.
The infection can progress rapidly, especially in immunocompromised individuals, making early detection and treatment essential.
Diagnosis of Invasive Aspergillosis
Diagnosing invasive aspergillosis can be challenging because its symptoms overlap with those of other infections. However, several diagnostic tools can help confirm the presence of Aspergillus infection:
- Medical history and physical examination: A doctor will assess risk factors, symptoms, and any relevant pre-existing medical conditions.
- Imaging: Chest X-rays or CT scans are often used to detect lung abnormalities caused by Aspergillus, such as nodules, cavities, or consolidation.
- Microbiological tests: A sample of sputum, blood, or tissue may be cultured to detect the presence of Aspergillus. However, cultures may not always be conclusive.
- Galactomannan test: A blood test that detects a substance released by Aspergillus fungi. Elevated levels can be a strong indicator of an Aspergillus infection.
- PCR (Polymerase Chain Reaction): This test can detect Aspergillus DNA in blood or tissue samples, providing a more sensitive and rapid diagnosis.
- Biopsy: In some cases, a tissue biopsy may be needed to confirm invasive aspergillosis.
A combination of these diagnostic methods is typically used to confirm the presence of invasive aspergillosis and determine its severity.
Treatment of Invasive Aspergillosis
Invasive aspergillosis requires prompt treatment to prevent the infection from spreading and causing severe complications. The primary treatment options are antifungal medications, and the specific approach depends on the severity of the infection and the individual’s overall health.
Antifungal Medications:
- Voriconazole: This is the first-line treatment for invasive aspergillosis. It’s a potent antifungal that works by inhibiting the growth of Aspergillus fungi.
- Amphotericin B: In severe cases, this potent antifungal may be used intravenously.
- Posaconazole or Isavuconazole: These are alternatives to voriconazole, especially in patients who cannot tolerate it or have resistance.
Surgery:
In some cases, surgical intervention may be required to remove infected tissue, particularly if the infection has caused abscesses or cavities in the lungs.
Supportive Care:
Supportive care, such as oxygen therapy, pain management, and treatment for secondary infections, may also be necessary, particularly in severely immunocompromised individuals.
Preventing Invasive Aspergillosis
Preventing invasive aspergillosis involves reducing exposure to the Aspergillus spores, particularly in high-risk individuals. Some preventive strategies include:
- Environmental controls: In hospitals and healthcare settings, air filtration systems can help reduce the number of airborne Aspergillus spores. Limiting construction work in healthcare environments can also reduce spore exposure.
- Protective measures: Immunocompromised patients may be advised to avoid dusty or moldy environments and wear protective masks when necessary.
- Prophylactic antifungal therapy: For patients undergoing chemotherapy, organ transplants, or bone marrow transplants, antifungal drugs may be prescribed as a preventive measure.
Final Thoughts
Invasive aspergillosis is a serious fungal infection that can have life-threatening consequences, especially for individuals with weakened immune systems. Early detection, accurate diagnosis, and timely treatment with antifungal medications are essential for improving outcomes. While prevention is challenging, careful management of risk factors and protective measures can significantly reduce the risk of developing invasive aspergillosis in vulnerable individuals.
If you or someone you know is at high risk for this condition, it’s important to stay informed, take preventive steps, and seek medical attention promptly if symptoms arise. With proper care and treatment, many individuals can recover and resume their normal lives.
The list of some Invasive Aspergillosis medicine:
Posanox
Posac
Xpos
Osapiderm DR