Our kidneys play a vital role in keeping the body balanced and healthy. They filter waste, regulate fluids, and control important hormones. When these organs are damaged, the consequences can affect many systems throughout the body. One of the most serious types of kidney damage is nephropathy, a condition that often develops gradually but can have lasting health impacts if left untreated.
Defining Nephropathy
Nephropathy is a general term used to describe damage or disease of the kidneys. It can result from a variety of causes and may affect how well the kidneys function. Over time, if not properly managed, nephropathy can lead to chronic kidney disease (CKD) or even kidney failure, requiring dialysis or a transplant.
There are several forms of nephropathy, each with distinct causes and effects. The most commonly discussed types include diabetic nephropathy, hypertensive nephropathy, and glomerulonephritis.
Types of Nephropathy
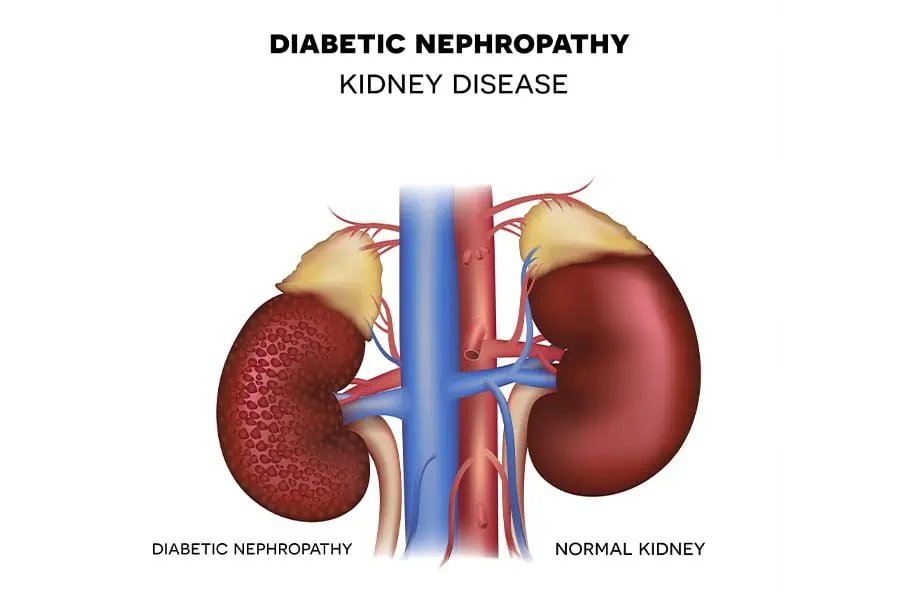
- Diabetic Nephropathy
This is one of the leading causes of kidney failure worldwide. High blood sugar levels in people with diabetes can gradually damage the blood vessels in the kidneys, making it harder for them to filter waste. It often develops over many years and may go unnoticed until significant kidney function is lost. - Hypertensive Nephropathy
High blood pressure can strain the kidneys over time, leading to damage of the blood vessels and filtration units. This type of nephropathy is especially common in people who have poorly controlled hypertension. - Glomerulonephritis
This involves inflammation of the tiny filtering units in the kidneys known as glomeruli. It can result from infections, autoimmune diseases, or unknown causes. - IgA Nephropathy (Berger’s Disease)
This condition occurs when the IgA antibody builds up in the kidneys, leading to inflammation and, eventually, kidney damage.
Symptoms of Nephropathy
In the early stages, nephropathy might not show any noticeable symptoms. As the condition progresses, symptoms may include:
- Swelling (edema) in the legs, feet, or hands
- Foamy urine due to excess protein (proteinuria)
- High blood pressure
- Fatigue
- Frequent urination, especially at night
- Decreased appetite
- Nausea or vomiting
- Confusion or trouble concentrating (in advanced stages)
Because kidney disease can be silent in its early stages, regular screenings are essential, especially for those at higher risk.
Risk Factors
Some of the most common risk factors for developing nephropathy include:
- Diabetes (especially type 1 and type 2)
- High blood pressure
- Family history of kidney disease
- Obesity
- Smoking
- Aging
- Certain autoimmune disorders, such as lupus
Managing these risk factors through lifestyle changes and medication can greatly reduce the chances of developing nephropathy.
Diagnosis and Testing
To detect nephropathy, doctors may use a combination of:
- Urine tests – to check for protein (albumin) or blood in the urine
- Blood tests – to measure creatinine and estimate kidney function (eGFR)
- Imaging tests – such as ultrasound or CT scans to view kidney structure
- Kidney biopsy – in some cases, a small tissue sample is taken to confirm the diagnosis and identify the specific type of kidney disease
Treatment and Management
While some forms of nephropathy cannot be completely reversed, they can often be managed to slow progression:
- Control of Underlying Conditions
- Properly managing diabetes and blood pressure is key to protecting kidney health.
- Medications such as ACE inhibitors or ARBs can help reduce kidney damage.
- Lifestyle Changes
- Eat a kidney-friendly diet low in sodium, protein, and processed foods.
- Stay active and maintain a healthy weight.
- Quit smoking and limit alcohol consumption.
- Monitor blood sugar and blood pressure regularly.
- Medications
- Diuretics to reduce swelling
- Drugs to lower blood pressure and reduce protein loss in urine
- In some cases, immunosuppressants for autoimmune-related nephropathy
- Dialysis or Kidney Transplant
In end-stage kidney failure, dialysis or transplant may be the only treatment options.
Preventing Nephropathy
While not all cases of nephropathy are preventable, early intervention can delay or prevent serious kidney damage. Here’s how to reduce your risk:
- Monitor chronic conditions like diabetes and hypertension closely.
- Drink enough water, but avoid excessive hydration.
- Avoid overuse of NSAIDs and other medications that can strain the kidneys.
- Get regular health checkups, especially if you’re at higher risk.
Conclusion
Nephropathy is a serious condition that affects the kidneys’ ability to filter waste and regulate the body’s fluid and chemical balance. While it can be progressive and potentially lead to kidney failure, early detection and proper management can help preserve kidney function and improve quality of life. By staying informed and proactive about your health, you can take important steps to protect these vital organs.
The list of some Nephropathy medicine:
Luciseta