Imagine constantly feeling the urgent need to rush to the bathroom—whether you’re at work, in the middle of a conversation, or asleep at night. For millions of people around the world, this is not just an inconvenience; it’s a daily reality. This condition is known as Overactive Bladder (OAB), and while it’s common, it’s often underreported due to embarrassment or misunderstanding.
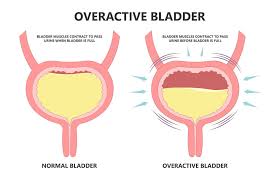
Overactive Bladder is a group of symptoms related to bladder control. It involves a sudden, uncontrollable urge to urinate—even when the bladder isn’t full. This urge may be difficult to suppress, and in many cases, it can lead to urge incontinence, or involuntary leakage of urine.
The key symptoms include:
- Urgency: A sudden, strong urge to urinate
- Frequency: Needing to urinate more than eight times in a 24-hour period
- Nocturia: Waking up two or more times at night to urinate
- Urge incontinence: Unintentional loss of urine immediately after an urgent need to go
What Causes Overactive Bladder?
OAB occurs when the bladder muscles contract involuntarily, even when the bladder isn’t full. This can be triggered by several underlying causes, including:
- Neurological conditions (e.g., multiple sclerosis, Parkinson’s disease, stroke)
- Urinary tract infections
- Bladder abnormalities, such as tumors or stones
- Hormonal changes, particularly after menopause
- Diabetes
- Certain medications or excessive caffeine intake
- Unknown causes, in which case it’s referred to as idiopathic OAB
While both men and women can experience OAB, it is more prevalent in older adults and tends to impact women more frequently.
How Is Overactive Bladder Diagnosed?
Diagnosing OAB begins with a detailed medical history and physical examination. Your doctor may also recommend:
- Urine tests: To rule out infections or blood in the urine
- Bladder diary: Tracking urination patterns for a few days
- Urodynamic testing: Measuring pressure and volume within the bladder
- Post-void residual test: Checking if the bladder empties completely after urination
These assessments help differentiate OAB from other conditions like urinary tract infections or prostate problems in men.
Treatment Options for Overactive Bladder
Fortunately, OAB is manageable. Treatment often starts with lifestyle changes, then progresses to medications or more advanced options if needed.
1. Behavioral Therapies
- Bladder training: Delaying urination gradually to increase bladder capacity
- Pelvic floor exercises (Kegels): Strengthening muscles to control urination
- Scheduled voiding: Urinating at set times rather than waiting for the urge
- Dietary changes: Limiting caffeine, alcohol, and spicy foods
2. Medications
- Anticholinergics and beta-3 adrenergic agonists: Help relax bladder muscles and reduce urgency
- Topical estrogen (for postmenopausal women): May improve symptoms related to vaginal and urinary tract tissue thinning
3. Advanced Treatments
- Botox injections: Temporarily paralyze bladder muscles to reduce contractions
- Nerve stimulation: Using mild electrical impulses to improve bladder control
- Surgery (rare): Considered for severe cases unresponsive to other treatments
Living with OAB: Tips for Daily Life
While OAB can affect emotional well-being and social interactions, many people manage it effectively with the right strategies. Here are a few tips:
- Wear absorbent pads for peace of mind during outings
- Know restroom locations when you’re out and about
- Stay hydrated, but avoid drinking large amounts all at once
- Talk openly with your healthcare provider—OAB is common and treatable
Conclusion
Overactive Bladder is more than just an inconvenience—it can interfere with sleep, work, and quality of life. The good news is that help is available, and the condition can often be managed through a combination of lifestyle changes, medications, and, if necessary, medical procedures. If you or someone you know is experiencing OAB symptoms, don’t hesitate to seek professional guidance. Early intervention can lead to better outcomes and restore control and confidence.
The list of some Overactive Bladder medicine:
LuciVibe