Cachexia is a multifactorial syndrome characterized by severe weight loss, muscle wasting, and fatigue. It is commonly seen in individuals with chronic conditions such as cancer, heart failure, kidney disease, and severe infections. Cachexia is more than just malnutrition—it’s a complex, systemic condition that cannot be fully reversed by nutrition alone, and it often leads to significant physical decline and poor quality of life.
In this blog, we’ll explore what cachexia is, its causes, symptoms, diagnosis, and treatment options, helping you better understand this often-overlooked condition.
Cachexia is a condition characterized by extreme weight loss, muscle wasting (sarcopenia), and significant fatigue, despite adequate caloric intake. Unlike simple malnutrition, cachexia cannot be fully reversed by increasing calorie intake alone. It involves changes in the body’s metabolism, including inflammation, hormonal imbalances, and alterations in protein and fat metabolism.
Cachexia is often associated with severe chronic diseases, particularly those involving inflammation, such as cancer, heart failure, and chronic kidney disease. The muscle and fat loss that occurs in cachexia can lead to weakness, fatigue, and a decrease in functional ability, which significantly impacts the individual’s quality of life.
Causes of Cachexia
Cachexia is not a disease itself but a consequence of various underlying conditions. Several factors contribute to the development of cachexia:
1. Cancer
Cachexia is most commonly seen in individuals with advanced cancer, particularly those with cancers of the digestive system (such as pancreatic, stomach, or colorectal cancer). The presence of tumors triggers a systemic inflammatory response that increases metabolic activity and alters the body’s ability to utilize nutrients, leading to muscle wasting and fat loss.
2. Heart Failure
Heart failure, particularly when it reaches advanced stages, can lead to cachexia. Chronic inflammation and decreased blood flow to tissues contribute to muscle loss. Additionally, heart failure often comes with other comorbidities like malnutrition, which can exacerbate the condition.
3. Chronic Kidney Disease (CKD)
People with CKD may develop cachexia due to the combined effects of poor nutritional intake, inflammation, and metabolic changes related to kidney dysfunction. Dialysis patients, in particular, are at higher risk for cachexia due to nutrient losses during treatment and the body’s inability to properly regulate metabolic processes.
4. Chronic Inflammatory Diseases
Conditions such as rheumatoid arthritis, chronic obstructive pulmonary disease (COPD), and sepsis can cause inflammation in the body, leading to cachexia. Chronic inflammation interferes with normal metabolism and nutrient utilization, contributing to muscle wasting and fat loss.
5. Neurological Diseases
Some neurological conditions, including amyotrophic lateral sclerosis (ALS) and Parkinson’s disease, can lead to cachexia. Muscle wasting is often a consequence of the progressive loss of muscle function and control, combined with altered metabolic processes.
6. Endocrine Disorders
Certain hormonal imbalances, such as those seen in hyperthyroidism or adrenal insufficiency, can contribute to cachexia. The hormonal changes lead to alterations in metabolism and fat storage, contributing to weight loss and muscle wasting.
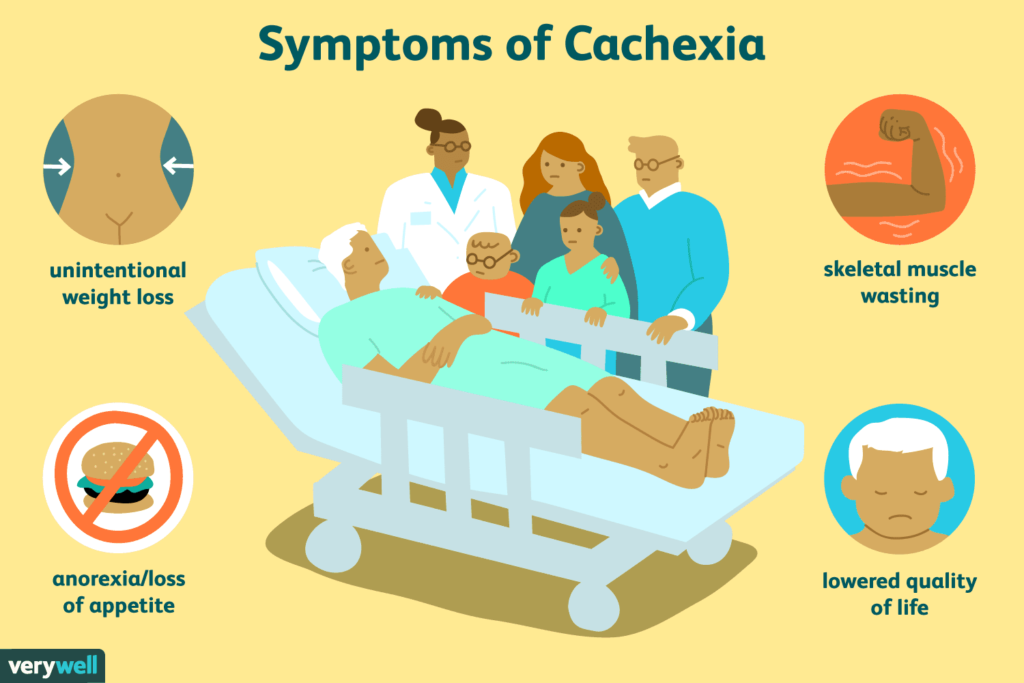
Symptoms of Cachexia
Cachexia is more than just weight loss. It includes a number of symptoms that can significantly affect a person’s physical and emotional well-being:
- Severe Weight Loss: This is often one of the most noticeable symptoms, particularly the loss of lean muscle mass rather than fat.
- Muscle Wasting (Sarcopenia): Muscle mass is broken down due to changes in metabolism, leading to weakness, fatigue, and difficulty performing everyday activities.
- Fatigue and Weakness: As muscle mass declines, individuals often experience extreme fatigue and lack of energy, which can make even simple tasks feel exhausting.
- Loss of Appetite (Anorexia): A common symptom in cachexia, decreased appetite is often caused by the underlying disease, hormonal changes, and inflammation.
- Increased Metabolic Rate: The body’s metabolism is often accelerated in cachexia, leading to the depletion of fat and muscle stores.
- Difficulty Breathing: In severe cases, muscle wasting can affect respiratory muscles, making it harder to breathe.
- Impaired Immune Function: Cachexia can impair immune function, increasing susceptibility to infections.
Diagnosing Cachexia
Diagnosing cachexia typically involves assessing the individual’s medical history, symptoms, and the underlying conditions contributing to the syndrome. Diagnostic tests may include:
- Body Composition Analysis: To assess muscle and fat loss, body composition can be measured using methods such as bioelectrical impedance analysis (BIA) or dual-energy X-ray absorptiometry (DEXA).
- Blood Tests: To evaluate levels of inflammatory markers (such as C-reactive protein) and other relevant biomarkers that may indicate an inflammatory process.
- Nutritional Assessment: A detailed review of the individual’s nutritional intake, including the assessment of calorie and protein consumption, can help determine if malnutrition is contributing to cachexia.
- Clinical Evaluation: A doctor will also assess symptoms such as weakness, fatigue, and changes in weight or muscle mass.
It’s important to recognize that cachexia may not be immediately obvious, especially in the early stages. It may develop slowly, making early detection and intervention crucial for managing the condition effectively.
Treatment Options for Cachexia
While there is no cure for cachexia, treatment focuses on managing the underlying condition, improving nutritional intake, and addressing symptoms to improve quality of life. Treatment plans often require a multidisciplinary approach, involving physicians, nutritionists, and physical therapists.
1. Nutritional Support
Increased caloric intake and protein supplementation are key components of managing cachexia. A high-protein, high-calorie diet is often recommended, along with the use of oral nutritional supplements (such as protein shakes) to help maintain weight and muscle mass. However, in severe cases, parenteral (IV) nutrition may be necessary if oral intake is insufficient.
2. Pharmacological Treatments
Several drugs can help reduce inflammation and promote weight gain in individuals with cachexia:
- Appetite Stimulants: Medications such as megestrol acetate or cannabinoids can help increase appetite, particularly in individuals with cancer or HIV/AIDS-related cachexia.
- Anti-Inflammatory Drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs) or corticosteroids may be used to reduce inflammation, which can help alleviate some of the metabolic changes contributing to muscle wasting.
- Anabolic Agents: Medications like anabolic steroids or selective androgen receptor modulators (SARMs) may help stimulate muscle growth and reduce the loss of lean muscle mass.
3. Exercise and Physical Therapy
While exercise alone cannot reverse cachexia, physical therapy and resistance training can help improve strength, reduce fatigue, and prevent further muscle loss. Tailored exercise programs designed to improve muscle function and endurance can play an important role in the management of cachexia.
4. Addressing the Underlying Condition
Managing the underlying condition that is causing cachexia is essential. This may involve chemotherapy for cancer, optimizing treatment for heart failure, or managing infections or inflammatory diseases. Treating the root cause of cachexia can help alleviate some of the symptoms and improve overall prognosis.
5. Psychosocial Support
Cachexia often impacts emotional well-being, so counseling and psychological support can be valuable for individuals and their families. Addressing depression, anxiety, or body image concerns is an important aspect of comprehensive care.
Conclusion
Cachexia is a complex and challenging condition that often arises in individuals with chronic diseases. While it cannot always be fully reversed, early recognition and comprehensive management can improve the quality of life and help individuals better cope with the physical and emotional effects of the syndrome. By focusing on nutrition, inflammation control, and appropriate medications, it’s possible to manage cachexia and help individuals maintain strength and function for as long as possible.
The list of some Cachexia medicine:
Megestol Suspension
Mezest
Apit
LuciAnam
Meganor
Mezoxia
Adlumiz